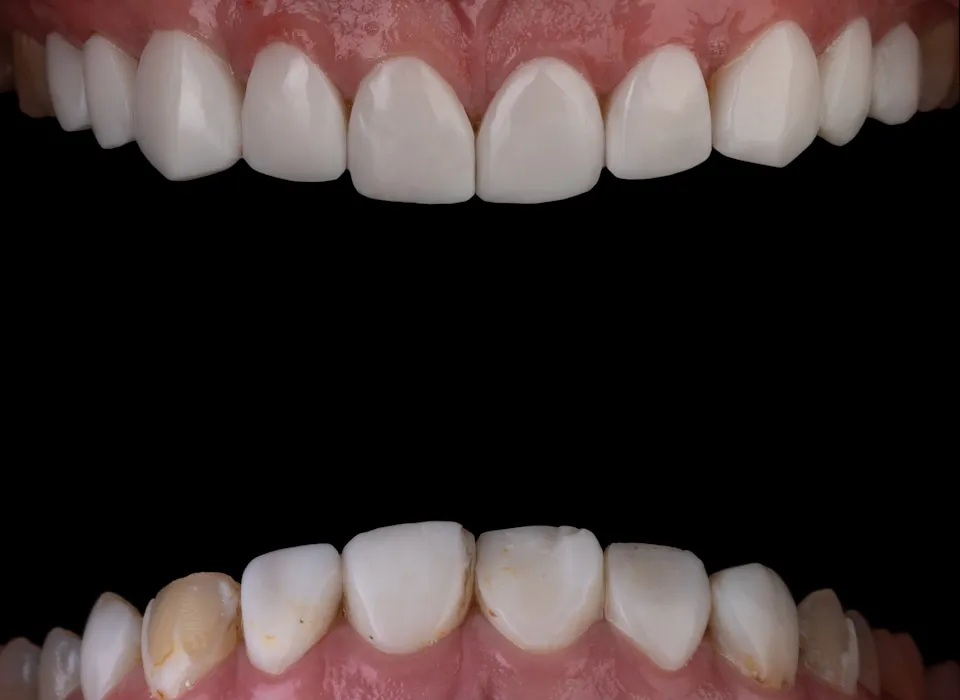
Cavities are the most common chronic disease in the world, yet most people do not fully understand how they form. After more than 45 years of treating patients in Huntington Beach, I can tell you that the patients who understand the mechanics of tooth decay are the ones who get the fewest cavities.
This guide explains the science behind cavities, the risk factors, the different types of decay, and the practical steps you can take to prevent them.
The Science Behind Cavities: How Tooth Decay Actually Works
A cavity — called dental caries in clinical terms — is not caused by sugar alone. It is the result of a chain reaction that involves bacteria, food, acid, and time. Here is how the process unfolds.
Your mouth is home to hundreds of bacterial species. Certain strains, particularly Streptococcus mutans, thrive on sugars and starches. When these bacteria consume sugar, they produce acid that attacks your tooth enamel — the hard outer shell protecting each tooth.
Every time you eat or drink something sugary, an acid attack begins within minutes and lasts 20 to 30 minutes. The acid dissolves minerals from the enamel in a process called demineralization — a form of enamel erosion that happens at the microscopic level.
Your body fights back through remineralization. Saliva delivers calcium, phosphate, and fluoride to the enamel surface, repairing damage. When remineralization keeps pace with demineralization, teeth stay healthy. But when acid attacks happen too frequently — from constant snacking, poor hygiene, or dry mouth — demineralization outpaces repair, enamel breaks down, and a cavity forms.
Think of it as a tug-of-war: bacteria, sugar, and acid on one side pulling toward decay, and saliva, fluoride, and good hygiene on the other pulling toward health. Cavities happen when the decay side wins.
The Four Stages of Cavity Formation
Cavities do not appear overnight. They develop through a predictable progression, and understanding these stages helps you appreciate why early detection and regular dental visits matter so much.
Stage 1: White Spot Lesion
The earliest sign is a white or chalky spot on the tooth surface, indicating mineral loss while the surface remains intact. At this stage, the damage is reversible with fluoride treatment, improved brushing, and dietary changes.
Stage 2: Enamel Decay
If the white spot is not addressed, enamel breaks down until a hole forms. This is a true cavity. A dental filling is needed to remove decay and restore the tooth.
Stage 3: Dentin Decay
Beneath enamel lies dentin, a softer layer. Once decay reaches dentin, it spreads quickly. You may feel sensitivity to hot, cold, or sweet foods. A filling can still treat the cavity, though a larger restoration may be needed.
Stage 4: Pulp Involvement
If untreated, bacteria reach the pulp — the innermost part of the tooth containing nerves and blood vessels. This causes significant pain, infection, and potentially an abscess. Treatment requires a root canal or extraction. This is why waiting until a tooth hurts is the most expensive approach to dental care.
Risk Factors: Why Some People Are More Vulnerable
Not everyone faces the same level of cavity risk. Several factors influence your susceptibility to tooth decay.
Diet high in sugar and refined carbohydrates. Frequent consumption of sugary drinks, candy, cookies, and chips gives mouth bacteria a constant fuel supply. The frequency of sugar exposure matters even more than the total amount. On the flip side, certain nutrients actively protect your enamel — learn which ones in our guide to foods that strengthen teeth.
Poor oral hygiene. Inadequate brushing and flossing allows plaque to accumulate, giving bacteria a permanent home. Learning how to brush your teeth properly is one of the most impactful things you can do.
Dry mouth (xerostomia). Saliva is your mouth’s natural defense against acid. Medications, medical conditions, and mouth breathing can all reduce saliva flow, dramatically increasing cavity risk.
Tooth anatomy. Back teeth have deep grooves and pits that trap food and bacteria, which is why molars develop cavities far more often than front teeth.
Genetics. The thickness of your enamel, the shape of your teeth, and even the bacterial composition of your mouth are influenced by genetics. Some people are simply more predisposed to decay.
Age. Cavity risk peaks in childhood and again in older adulthood, when gum recession exposes root surfaces and medications cause dry mouth.
Existing dental work. Old or worn fillings can develop gaps where bacteria infiltrate. Decay beneath an existing restoration is called recurrent caries and is a common reason fillings need replacement.
Three Types of Cavities
Cavities are classified by their location on the tooth. Each type has different characteristics and risk factors.
Smooth Surface Cavities
These form on the flat exterior surfaces of teeth, usually where teeth contact each other. They develop slowly and respond well to fluoride treatment when caught early.
Pit and Fissure Cavities
These develop in the deep grooves on chewing surfaces of molars. They are the most common cavity type because grooves naturally trap food and bacteria. Dental sealants are extremely effective at preventing them, especially in children with newly erupted permanent molars.
Root Cavities
Root cavities form on exposed root surfaces after gum recession. Roots are covered by cementum, which is softer than enamel and decays more easily. They are most common in older adults and progress quickly.

How to Prevent Cavities: Proven Strategies
The good news about cavities is that they are largely preventable. Here are the most effective strategies, ranked by impact.
Brush Twice a Day With Fluoride Toothpaste
Fluoride strengthens enamel and enhances remineralization. Brush for two full minutes, reaching every surface. Use a soft-bristled brush and replace it every three months. For technique guidance, read our guide on how to brush your teeth properly.
Floss Daily
Brushing alone cannot reach the tight spaces between teeth where cavities frequently develop. If traditional floss is difficult, water flossers and interdental brushes are effective alternatives.
Limit Sugar Frequency
Pay attention to how often you consume sugar, not just the amount. Sipping a sugary drink over two hours causes continuous acid attacks. Drinking it in ten minutes causes one shorter attack. Minimize snacking between meals.
Get Dental Sealants
Dental sealants are thin coatings applied to the chewing surfaces of molars, reducing cavity risk by up to 80 percent. They are commonly placed on children’s permanent molars, but adults with deep grooves can benefit as well.
Use Fluoride Strategically
Beyond fluoride toothpaste, your dentist may recommend professional fluoride treatments or prescription-strength fluoride toothpaste if you are at elevated risk for decay.
Stay Hydrated and Address Dry Mouth
Drink water throughout the day to support saliva production. If you take medications that cause dry mouth, talk to your dentist about strategies to restore moisture and protect your teeth.
Visit Your Dentist Regularly
Professional cleanings remove hardened plaque that your toothbrush cannot. Dental exams with X-rays catch cavities in their earliest stages, often before you feel any symptoms. Learn more about scheduling in our article on how often you should visit the dentist.
Treatment Overview: What Happens When You Get a Cavity
If a cavity is detected, treatment depends on the stage of decay.
- White spot lesions may be treated with fluoride applications and monitoring
- Small to moderate cavities are treated with composite (tooth-colored) fillings
- Large cavities may require an onlay or crown to restore the tooth’s structure
- Deep decay reaching the pulp requires root canal therapy followed by a crown
- Severely damaged teeth that cannot be saved may require extraction and replacement with a dental implant or bridge
The earlier a cavity is caught, the simpler and more affordable the treatment. This is the strongest argument for keeping your regular dental appointments even when nothing hurts.
Why Early Detection Changes Everything
I have spent over four decades telling patients the same thing: the best time to treat a cavity is before you know it is there. By the time a cavity causes pain, it has usually progressed to the dentin or pulp, requiring more extensive and costly treatment.
A cavity caught as a white spot lesion may not need any drilling at all. A small cavity caught during a routine exam can be filled in a single, comfortable appointment. But a cavity ignored for months or years can lead to infection, tooth loss, and thousands of dollars in restorative care. Prevention and early detection work together — the habits you practice at home reduce your risk, and the appointments you keep at our office catch what your home care misses.
Protect Your Smile Starting Today
Understanding what causes cavities gives you the power to prevent them. If it has been more than six months since your last dental visit, or if you are experiencing sensitivity, discomfort, or visible changes in your teeth, do not wait for the problem to grow.
Call HB Dentist today at (714) 964-4183 or schedule your appointment online. Dr. Baldwin and our team in Huntington Beach are here to help you stay cavity-free for life — and it starts with your next visit.